
Today was hard. I had to take my middle son, Lucas for a chest X-ray and as it turns out, the persistent cough that keeps making him gag and vomit, is actually pneumonia.
Today was especially hard though, not just because of the diagnosis, but because it reminded me of the time he almost died.
Having this happen today made me want to write about medical trauma, because so many people don’t realize that they have ever experienced it despite its prevalence; making it especially important for those of us with sexual trauma to understand, unpack, and process what we have been through.
You may be wondering…
‘Medical trauma’ refers to a set of physiological and psychological responses that occur as a result of single or multiple medical events.
It is in essence a traumatic response to events, brought on by an intense emotional experience during which we feared for our own safety or the safety of a loved one.
‘Medical trauma’ can include a wide range of experiences from any kind of hospitalization, as well as fractures, wounds, strong physical allergic reactions, surgeries, poisoning, burns, pre and peri-natal trauma, the list goes on and on.
It’s important to reiterate that it doesn’t have to be from our own experience. For example, if you are visiting a sick relative at the hospital, or if a loved-one is hospitalized after a motor-vehicle accident, or for a surgery, there can be all sorts of trauma responses associated with these events that will need careful time and attention to process and heal.
If you find yourself having a strong emotional or physical (somatic) reaction when you think about going to see a doctor, or dentist, or going to a hospital or any other medically related place, then it’s likely that you may have experienced some medical trauma. For example, if your palms sweat and your heart races whenever you see an ambulance, this may indicate that there is some healing to be done.
You may be thinking to yourself ‘Sure, I don’t like doctors, dentists or hospitals. But who does? Why should this matter to me?’
Here’s why…
#1 – If you want to understand sexual trauma better and how to heal from it, it’s important to also understand medical trauma, and the ways that different categories of trauma can stack and interweave with one another. Understanding this stacking effect is especially important for those of us with sexual trauma because of the inherent threat to personal safety that is so common within both categories of trauma.
#2 – Visiting a doctor, dentist or hospital is something we’ll all have to do again at some point. And if we let medical traumas stack without understanding or healing them, (especially if we’ve had very strong experiences), it may be very limiting to our sense of safety and our ability to be in these environments without experiencing massive psychological and physiological discomfort.
To help you understand more, let me tell you a bit about my son’s medical trauma and how it affected me. I think through reading this story, you’ll understand, and more importantly feel, just how medical trauma may be impacting you.
 Like I said, today was hard because I had to take my son for a chest X-ray.
Like I said, today was hard because I had to take my son for a chest X-ray.
As we bundled up, left the warmth of my car and trudged across the icy parking lot, my ever-so-cool, almost 9 year old tucked his arm through mine and leaned his head against my shoulder.
My heart plummeted. My happy-go-lucky kid has never been a complainer and these public snuggles only ever show up when he’s feeling truly unwell.
We made it inside and joined the back of a long line in the radiology department. As we stood there, not quite patiently waiting for our turn to fill out paperwork, I cast my gaze around and let my senses take in the room. The clinically-clean citrus smell, the drab and dated striped decor, the anxious and fearful look in people’s eyes; everything reminded me of back then. It was like opening the door to a chapter closed long ago.
In an instant I was reminded of all the hours, days, weeks and months spent, driving my mother back and forth to endless tests and rounds of radio and chemo cancer treatments.
As we waited, I watched the bustling comings and goings of the staff, acutely aware of the avalanche of emotions perilously close to overtaking me.
But today was not about her, or this unexpected fresh wave of grief, it was about my son. And so, with a silent prayer and a very long, slow, deep intake of breath, I pulled myself back to the present.
As we sat there in the sterile hardback chairs, waiting for our turn, we started a game of I spy. But Lucas was disinterested and weary and so we retreated into silence. He closed his normally boisterous eyes and sank against me. I began to pray. ‘Thank you God for keeping Lucas safe. Thank you for watching over him. Thank you for helping him return to good health quickly. And thank you for sending me a sign that everything is going to be ok’.
Like I said, I pray. A lot!

Eventually Lucas’ name was called and we followed the nurse technician along the labyrinthine corridors to the X-ray department. She showed us into a tiny cubicle changing room and handed me a miniature gown for him to put on, but the cartoon tigers on it made me sad. As I tied the back straps, I prattled on, chatting inanely about school and Christmas and video games. Anything to keep the mood light and the desolation I was feeling at bay.
The technician returned pretty quickly and escorted us to the X-ray room. She lined up the X-ray grid on Lucas’ back as he stood there hugging the giant cold machine. She asked me to leave on account of the radiation and closed the door.
Alone in the corridor, my eyes welled up with tears and I allowed myself to remember. I remembered the pain and the fear; the panic and helplessness of almost losing him when he was just 15 months old.
Unfortunately, this is what happens with medical trauma. It stacks, it compounds, it merges, overlaps and over-couples with other traumas.
And so, going for an X-ray was not just about going for an X-ray. It brought with it not only the usual mom-stress of worrying about and caring for a sick child, but also all the other similar incidents that were stored and flagged within my Nervous System.
That is, after all, the job of our Nervous System and in particular, the amygdala. Like sorting through a massive filing-cabinet, my amygdala found a folder marked ‘medical trauma’.
Immediately and unconsciously it pulled up every reference to my mother’s cancer treatment as well as my son’s complicated and extensive medical history. It brought up all the grief of losing my mother so young and it brought up all the fear and guilt and helplessness that I had felt back then when my son was a baby. Had I done enough? Was it all my fault? What if he’d died? Would he be emotionally scarred too?
What difficult medical experiences have you had?
Take a moment to think about your own experiences with medical trauma. Have you ever been hospitalized? What were the circumstances? How did you feel before, during and after? Did you heal quickly? Did you experience strong emotions or the absence of them? Were there other traumas that this experience brought up for you? And what about your loved-ones? Have you ever visited them in hospital? If so, how did that make you feel? Were you fearful, anxious or stressed? Have you ever lost a friend or loved-one following a medical procedure, surgery, accident, illness or injury? How did you respond? Did you experience guilt or blame yourself in some way for what happened? Were you able to grieve?

So there I was, waiting for the X-ray to be taken, but I wasn’t really there at all, I was back then – back when Lucas was just 15 months old. Because of all of his allergies and inability to properly digest and absorb nutrients, Lucas became malnourished.
He developed edema (swelling) in his hands and feet, double pink eye and double ear infections. He woke up crying and it was a cry I’d never heard before. I ran in to his room to find him standing in his crib with his eyes gummed shut, unable to see. I scooped him up and his pitiful whimper let me know something was badly wrong.
I brought him straight to the doctor, but Lucas was becoming increasingly lethargic and unresponsive. He was limp and dehydrated. The doctor told me to bring him straight to the hospital. I called my husband, Alex and he met us there.
Things deteriorated rapidly. They wanted to rule out meningitis and insisted on doing a lumbar puncture. On my baby! I was terrified but met their insistence with equal determination. If they were going to stick a gigantic needle in my baby, I, not some stranger, would be the one holding him.
The intensity of that moment will be forever etched on my heart. Locking eyes with the doctor, restraining and bracing Lucas’ tiny arms and legs whispering ‘I’ve got you baby, Mummy’s here, you’re safe’. Time stopped as the needle was inserted; the doctor missed the pocket of spinal fluid and the the syringe filled with blood. All that pain for nothing. I was devastated. The results were inconclusive and now we had to wait for the labs to culture the sample.
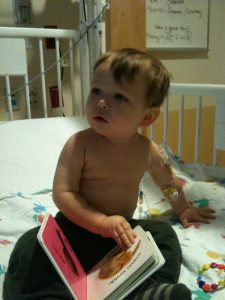 The ER medics decided Lucas needed to be transferred to a special children’s unit an hour away. Seeing his tiny body hooked up to all these machines, wearing a tiny oxygen mask made my blood run cold.
The ER medics decided Lucas needed to be transferred to a special children’s unit an hour away. Seeing his tiny body hooked up to all these machines, wearing a tiny oxygen mask made my blood run cold.
Riding alongside him in the ambulance, holding his hand and soothing him with my voice was all I could think of to do. His stats were not good. The paramedic looked concerned. I prayed and prayed the entire siren-blaring ride. I could see my husband’s car weaving in and out of traffic behind us, desperately trying to keep up as we sped along.
The next seven days were a total sleep-deprived blur. Because of the inconclusive meningitis results, and the possibility that he might be contagious, we had to stay in droplet quarantine in the ICU. No family could visit, not even my older son, and every member of staff wore full masks, gowns and gloves at all times. They wanted us to do the same but we declined. If things did go as badly as we feared, we wanted to be there to love and comfort, not scare our baby.
We spent fitful nights taking turns holding Lucas in our arms as he slept. Being that close to us was the only way he would rest. We rotated between a tiny sofa and a child sized cot. Endless streams of doctors and interns and medical students came and went twenty-four hours a day. Being that the children’s ICU unit was part of a teaching hospital, Lucas naturally became a human pin-cushion with them taking test after test, and blood after blood; replacing it with fluids from a bag. We felt so powerless and out of control to help our baby.
No tests were conclusive and no one could give us any answers about why our son was so terribly ill. The doctors made all kinds of wild hypothesis, even insisting at one point that he needed to be put on Thyroid medication for life.
We felt so very helpless and afraid. Who were we to know what would save our son’s life? Surely the doctors knew best? But it didn’t feel like that at all. We followed our gut instinct and found ourselves fending off medical interventions one after another. His levels were all well out of range, but we fought to let his condition stabilize before making any rash decisions about life-long treatment plans.
Slowly but surely Lucas’ vitals improved. His eye and ear infections cleared up, he was fully re-hydrated and alert and his test levels re-balanced. A week and a lot of arguments later, Lucas was finally sitting up, playing with the little train set his daddy had brought from home. He even managed a smile when we told him we could go home. We were so relieved.
I was yanked back from my memory as the X-ray room door swung open; wiping my eyes as Lucas re-joined me in the hallway. The nurse told us that the results had been ordered STAT and that the Radiographer would read the X-ray right away.
Lucas dressed and before long we were out in the dazzling snow-reflected daylight, making our way back to the car.
To my pleasant surprise, Lucas’ specialist called before we even made it out of the parking lot. He confirmed that it was pneumonia and called in the meds which I gladly picked up on our way home. An hour later, we were sitting at the kitchen table, facing – off in an intense game of Battleships. It felt good to just be together doing something so normal.
Later that night, after the kids went to bed, I took time to reflect on the day and on how much the whole experience had brought up for me. Why had all those memories come flooding back to me as I stood there in the radiology department hallway? Why was I reminded of my mother’s illness and treatment all those years ago? Hadn’t I done enough to heal my grief, my fears and feelings of helplessness? And had I done enough to help Lucas release the trauma and move on too? Or was his nervous system still stuck back then?
In the 7 years since Lucas’ time the ICU, I have done so much to heal for him and for me too.
I have grieved. I have sat with my fears and the helplessness. I have Tapped and journaled and used SE techniques. But as with all healing work, there is always another layer of the onion to be peeled; another strand of spaghetti to be untangled.
Do I feel bad that today brought up so much for me? Do I feel like I’m failing to heal or that I’m moving too slowly? No, I don’t. Medical trauma is extremely complex and I am choosing to give myself all the time and space that I need to feel all of my feelings. Yes this brought up a lot. It brought up the loss of my mother and possible loss of my son. Those are big traumas.
The more times we have to recount a medical history in a doctor’s office the harder it can be to release the intensity of emotions surrounding it. Over the years, I have had to tell and re-tell his history on countless occasions. It took me a long time to see or hear an ambulance without having a panic attack for example, but with Tapping and SE work, I have been able to release a great deal of the charge that his story has. No I can never change the event itself. I can’t turn back the clock, but little by little I can release more and more of the pain and suffering that remembering the event brings.

I have spent a great deal of time working with Somatic Experiencing (SE) to help him to re-negotiate the trauma; to allow his body to push against me and imagine escaping the lumbar puncture, and all the needles and tests. I’m not sure how much there is still for him to process, but I do trust that he is on his own journey.
He has grown into a funny, gregarious kid who is larger than life and in the very top of his grade at school. But without a doubt, that whole experience; those days in the ICU changed him. He has a depth and perspective on life that stretches far beyond his years. A gratitude and appreciation for the very fact that he survived and a wisdom that still catches me off guard at times.
If you’ve experienced medical trauma in your life, then reading my story today may have brought up and made you feel the emotions of those experiences all over again. If so, it’s important to understand why.
When we think about medical trauma, it’s important to understand that any time we combine fear with immobility, we create the perfect conditions for trauma.
In the case of medical interventions, there are all sorts of opportunities for a person to find themselves immobilized and to feel like the situation (or threat) is inescapable. For example, they might be strapped to a gurney and unable to get up. They might be hooked up to heart-rate monitors or an IV drip. They may be anesthetized during a surgery or partially immobilized in a neck brace, splint or cast.
Illnesses and injuries are unusual also, in that the threat comes from an internal, not an external source. This can create great confusion within a person’s nervous system. The nervous system wants to take defensive action, but there is no external threat like a tiger or a bear to fight or run from.
When a person cannot fight and cannot flee, but there is tremendous fear and activation in the nervous system, the stress hormones in the body eventually reach an intolerable (threshold) level and shut down; freeze becomes the default state and it is with this state that we must work when we are healing from medical trauma.
So, what can you do if you’ve experienced medical trauma in your life? What steps can you take to release the pain and suffering you experience around the event?
Step 1: Break the experience down in to tiny manageable pieces that can be safely worked with and Tap on the different pieces.
All too often, we can be overwhelmed and re-traumatized when we attempt to work with a trauma in one big piece. It is essential to break it down. Perhaps you might want to first give the event a headline like ‘car accident’. Notice the intensity that you feel when you just think about the headline title of the event.
You can use EFT Tapping to reduce this intensity. Only when the intensity is down as low as you can get it – preferable to around a 2 or a 3, should you move on to working with the next tiny piece of the event.
Step 2: Process the event using the ‘movie technique’
Repeat the process for step 1, but this time start way before the traumatic event occurred. Go back before anything happened.
Imagine that you are in a movie theater. You are up in the control room. You notice a large remote control with a red button on it. You pick up the remote. You see it in your hand. How does it feel? Is it cold to your touch? You are in control.
Very far away, down through the control room window, you see a movie screen. You notice that there is a movie paused on the screen. You have complete control over the movie. You can press play, stop, pause, re-wind and fast-forward – at any time.
Now, when you are ready, very slowly move forwards through the movie of your traumatic event. Pause any time there is ANY intensity at all. When you notice that intensity, stop. Rate the intensity and then Tap. Tap on the feelings, emotions and sensations that arise. When you feel like the intensity is down again, you can continue forwards with the movie.
Repeat this in as many tiny pieces and stages as you need until your movie is complete and the charge around the traumatic event has decreased substantially.
Step 3: Seek help and support when needed
When you are working with medical trauma, it is extremely important to realize that a key hallmark of this kind of trauma is the freeze response. This means that we are much more likely to dissociate and ‘go offline’.
Our conscious, rational thinking brain or ‘frontal-cortex’ will be unavailable. This means that working through this kind of trauma alone can be very challenging. As ever, I thoroughly recommend that you reach out to a practitioner who can support you as you process through your medical trauma.
If you would like to work with me one-on-one, you can find out more by going here.
